
You recovered from COVID. You felt mostly fine. But something is still off — certain foods taste wrong, or smell like garbage, or you can’t taste anything at all. And you’re starting to wonder if this is just… permanent now.
You’re not alone, and you’re not imagining things. Persistent taste and smell disruption after COVID affects millions of Americans and is one of the most under-explained aspects of long COVID. Here’s what’s actually happening.
What COVID Does to Your Olfactory System
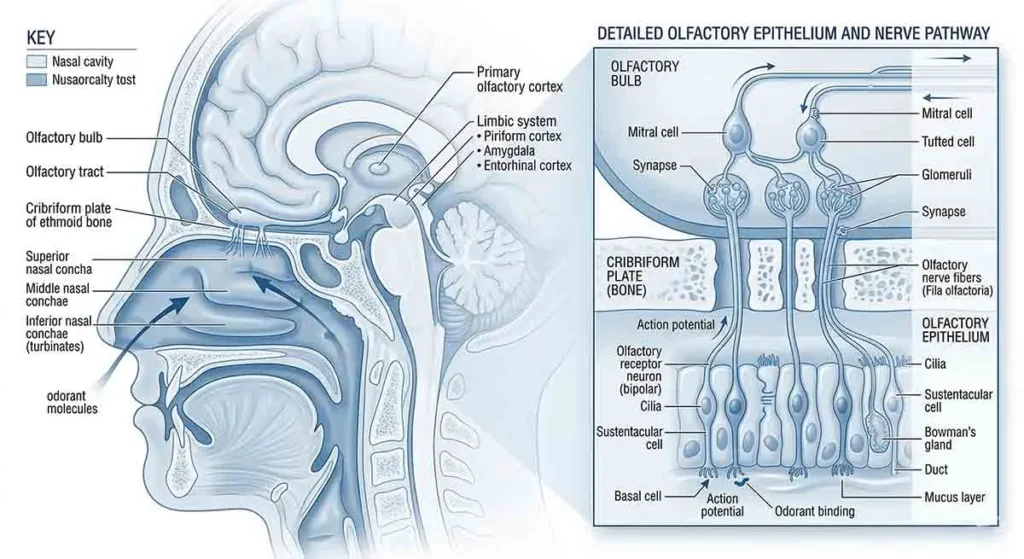
Your sense of smell (olfaction) is your most direct sense — olfactory neurons are the only neurons in your body that directly interface with the outside world without an intermediary. COVID-19, particularly earlier variants, had a strong affinity for the ACE2 receptors found in the supporting cells of the olfactory epithelium — the smell-sensing tissue inside your nose.
The virus damaged these supporting cells, which in turn disrupted the olfactory sensory neurons they maintain. For most people, this resolved. For an estimated 15–20% of COVID-infected individuals, the disruption persisted — sometimes causing complete smell loss (anosmia), sometimes causing distorted smell (parosmia), and sometimes causing phantom smells (phantosmia).
Because taste and smell are deeply integrated (most of what we experience as “flavor” is actually smell), damage to the olfactory system dramatically alters how food tastes even when the taste buds themselves are completely unaffected.
Parosmia: When Normal Smells Turn Wrong
Parosmia is the most distressing version of post-COVID smell disruption. Rather than simply losing smell, parosmia causes your brain to map smells to entirely wrong signals. The result: things that should smell good smell rotten, chemical, or foul.
Common parosmia triggers reported by post-COVID patients include: coffee (often described as smelling like garbage or sewage), meat, eggs, garlic, onion, and many fried or roasted foods. This is why some long-COVID patients lose significant weight — eating becomes an unpleasant or nauseating experience.
Foods Most Commonly Affected
Research from smell and taste clinics treating long-COVID patients has identified consistent patterns:
- Most commonly distorted: Coffee, meat (especially chicken), eggs, garlic, onion, alcohol, chocolate, roasted or fried foods.
- Often tolerated well: Plain carbohydrates (plain rice, plain pasta, bread), mild fruits, dairy products, cold or room-temperature foods rather than hot foods (heat releases more volatile aroma compounds).
- Sweet and salty tastes are often preserved because they rely on taste buds (not olfaction), while umami and complex flavors are most impacted.
What Recovery Actually Looks Like
The good news is that most people do recover — but the timeline is longer than expected and non-linear. Research published in peer-reviewed smell and taste journals suggests:
- Approximately 60% of those with parosmia see significant improvement within 12 months.
- Another 25–30% see gradual improvement over 18–24 months.
- A smaller percentage experience persistent disruption beyond two years, though even these cases often show some improvement with therapeutic intervention.
Recovery is rarely “one day it’s suddenly normal.” More typically, distorted smells gradually become less intense over months, specific triggers slowly improve, and the overall range of tolerable foods expands incrementally.
Strategies That Help
- Smell training. This is the most evidence-supported intervention. It involves intentionally smelling four specific scents (typically rose, lemon, eucalyptus, and cloves) twice daily for at least 12 weeks. Clinical trials show this significantly accelerates olfactory nerve recovery.
- Avoid your trigger foods without shame. There is no benefit to forcing yourself through a meal that tastes like chemicals. Focus on what you can tolerate and build from there.
- Cold or room-temperature foods. These release fewer volatile aroma compounds and are often more tolerable for parosmia sufferers.
- Nutritional supplements. Vitamin A (in recommended doses) shows some evidence for supporting olfactory epithelium repair. Alpha-lipoic acid has been studied with mixed but promising results.
- See a smell and taste specialist. These clinics exist at academic medical centers and are increasingly familiar with post-COVID presentations. A general practitioner will often have limited tools; a specialist can offer more targeted support.



Leave a Reply